Despite challenges, Quebec health-care workers adapting well to stress
- Salle de presse
02/03/2021
- UdeMNouvelles
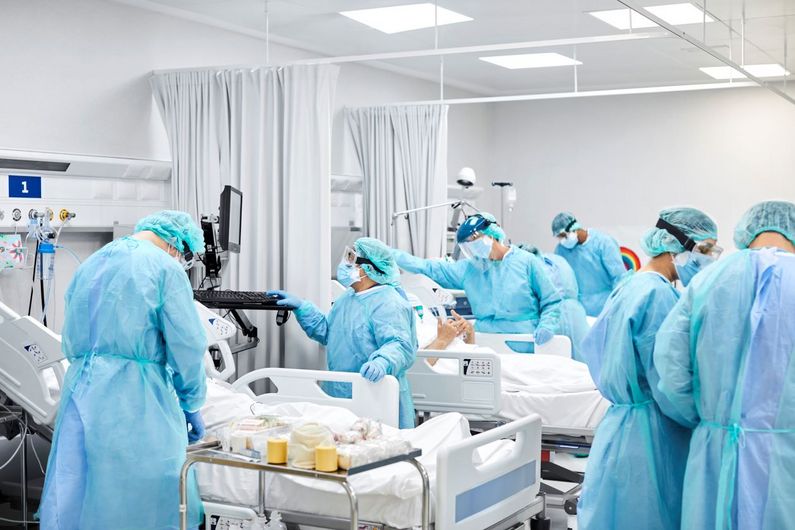
Eighty-five per cent of staffers in hospitals and long-term-care centres coped well with the mental stress they experienced during and after the first wave of the COVID-19 pandemic last year.
In a hospital or long-term-care centre, the stress felt by staff takes many forms: anxiety, insomnia, depression, psychological distress. To help gauge their well-being, in May 2020 a self-monitoring smartphone app was launched in Quebec by two Université de Montréal professors.
Now the preliminary data from those phones – collected by psychiatrist Nicolas Bergeron of the CHUM Research Centre and psychoeducator Steve Geoffrion of the Centre de recherche de l’Institut universitaire en santé mentale de Montréal – are in.
Presented today at a CHUM conference on suicide prevention, the professors’ analysis of the data provides a glimpse into what health-care workers went through psychologically during and after the first wave of the COVID-19 pandemic Iast spring and summer in Quebec.
Provided by close to 400 hospital and long-term-care centre staffers who used the app between May and September, the data suggest that “the majority of the people monitored have recovered well from the stressful experiences they may have had,” said Bergeron.
“For nearly 85 per cent of them, the distress they felt was transitory. In the specific context of COVID-19, our study is one of the first in the world to draw a longitudinal portrait of personal mental health.”
Preventing chronic stress
For their study, Bergeron and Geoffrion recruited 373 hospital staff – doctors, nurses, orderlies and others – at the CHUM (Université de Montréal’s teaching hospital), the CIUSSS de l’Est-de-l'Ile-de-Montréal and the CIUSSS of the Capitale-Nationale, in Quebec City. Each, the participants answered a series of questions on their phones about their psychological health, their exposure to major events and to stress, the support they received, and more.
The two researchers believe their study opens up new perspectives: how might medical teams better support people who work in their midst and are in distress? Should the accompaniment strategies offered internally by hospitals be adapted to different needs: group sessions, individual sessions, peer support, psychological first-aid? Further studies would be needed to answer these questions, the professors said.
“It remains essential to focus on health-care workers who did not show resilience and who experienced psychological distress during this first wave {of the pandemic},” said Geoffrion. “Preventive mental-health intervention in our institutions is also critical to prevent distress from becoming chronic.”
Help on the way
Various initiatives are already underway:
- Five other CIUSSS’s and CISSS’s, acronyms for Quebec’s university and integrated health and social-services centres, have adopted the use of the UdeM professors’ mobile phone application this winter, in the second wave of the pandemic.
- At the CHUM, the hospital’s psychology department has set up a program called Adapte-COVID to support employees during the pandemic. CHUM psychologists are available to listen to and help those in need.
- The CIUSSS de l’Est-de-l'Île-de-Montréal has a psychological first-aid program and a psychosocial support telephone line, and its employee-assistance program also offers services to family members of staff.
- Finally, all employees of the CIUSSS de l’Est-de-l'Île-de-Montréal have been invited to participate in Steve Geoffrion's COVID-19 100 Day Challenge and take a few minutes a day to measure how they are doing in several areas of their lives.
About this study
“Peur, confinement, fatigue et résilience : étude longitudinale sur la détresse psychologique des travailleurs de la santé pendant la pandémie au Québec,” by Nicolas Bergeron and Steve Geoffrion, was presented Feb. 3, 2021 at a conference organized at the Centre hospitalier universitaire de Montréal for the 2021 Quebec Suicide Prevention Week. Bergeron and Geoffrion were assisted in their study by co-researchers Stéphane Guay (Centre de recherche de l'Institut universitaire en santé mentale de Montréal) and Dr. Shelley-Rose Hyppolite (Direction de la santé publique du CIUSSS de la Capitale-Nationale). Their research was funded by the Fonds de recherche du Québec and the Ministère de l'Économie et de l'Innovation.
About the CRCHUM
The CHUM Research Centre (CRCHUM) is one of North America’s leading hospital research centres. It strives to improve the health of adults through a continuum of research spanning disciplines such as basic science, clinical research and population health. More than 2,150 people work at the CRCHUM, including nearly 500 researchers and nearly 650 students and postdoctoral fellows. crchum.com
About the CIUSSS de l'Est-de l'Île-de-Montréal
The Centre intégré universitaire de santé et de services sociaux de l'Est-de-l'Île-de-Montréal (CIUSSS-EMTL) encompasses 26 facilities and serves a population of more than 500,000 Montrealers. Affiliated with the Université de Montréal, it offers a complete range of frontline healthcare and social services, housing services, and general, specialized, and superspecialized hospital services and mental health care. Thanks to its two research centres and its four pillars of excellence in mental health, immuno-hematology, eye healthcare and nephrology, the CIUSSS-EMTL is a leader in health innovation in Canada. Its teams´ innovative ideas contribute to its national and international reach.
Media contact
-
Jeff Heinrich
Université de Montréal
Tel: 514 343-7593