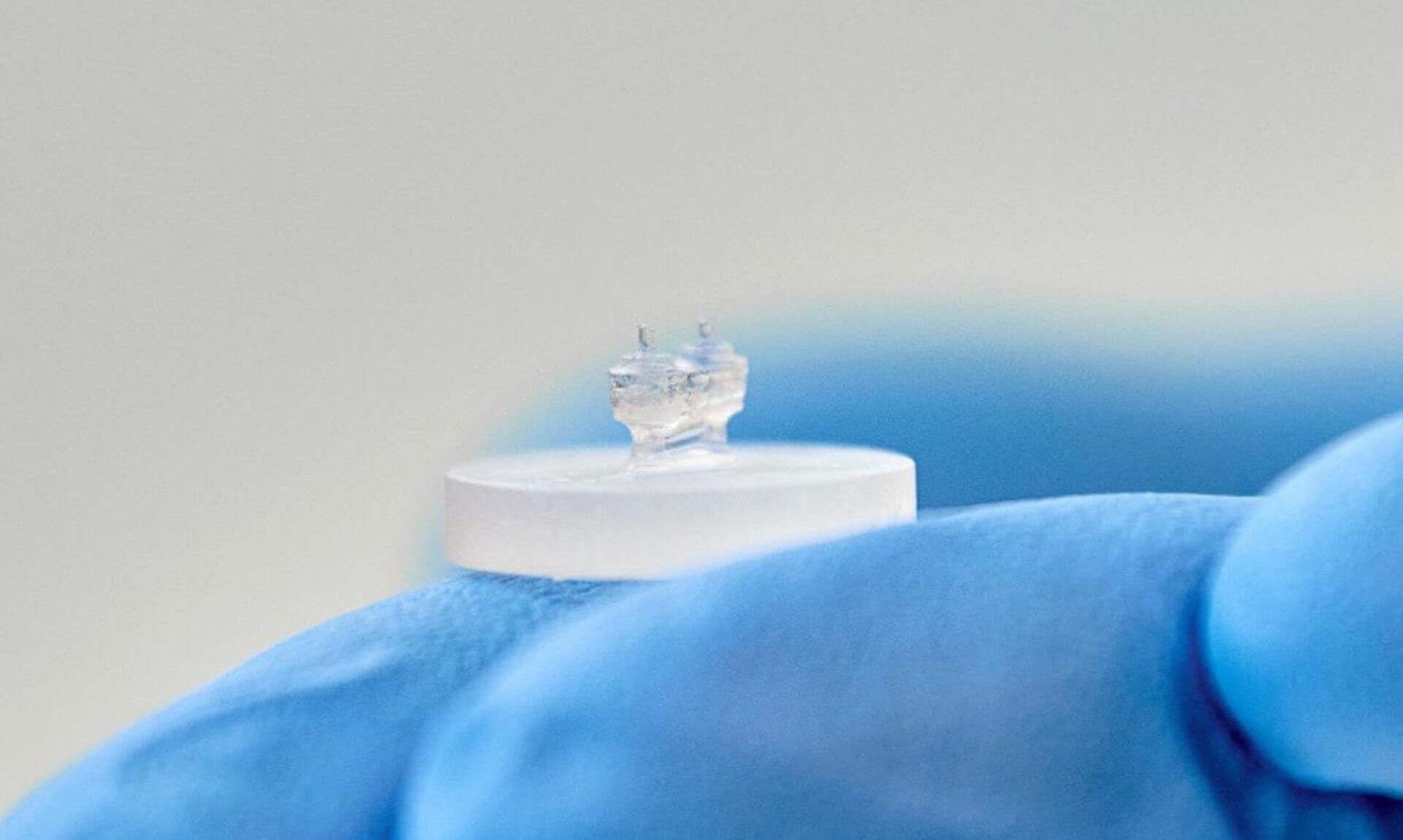
Scientists at Université de Montréal and its affiliated Centre de recherche Azrieli du CHU Sainte-Justine have made a major advance in their research into cardiovascular disease: they've created a functional, three-dimensional heart tissue that can beat autonomously in vitro.
The tissue incorporates micro-sensors that make it possible to do finely tuned, real-time analysis of its contractile properties. This advance marks an important step forward for modeling human cardiac diseases and conducting preclinical drug testing.
Led by UdeM pharmacology and physiology professor Houman Savoji at his laboratory at CHU Sainte-Justine, along with UdeM PhD student Ali Mousavi, the research is detailed in a study published in the scientific journal Nano Micro Small.